Revenue Cycle Management That Keeps Your Cash Flow Moving
AM Claims delivers revenue cycle management services that help providers reduce billing friction, improve reimbursement visibility, and strengthen financial performance from intake to final payment.
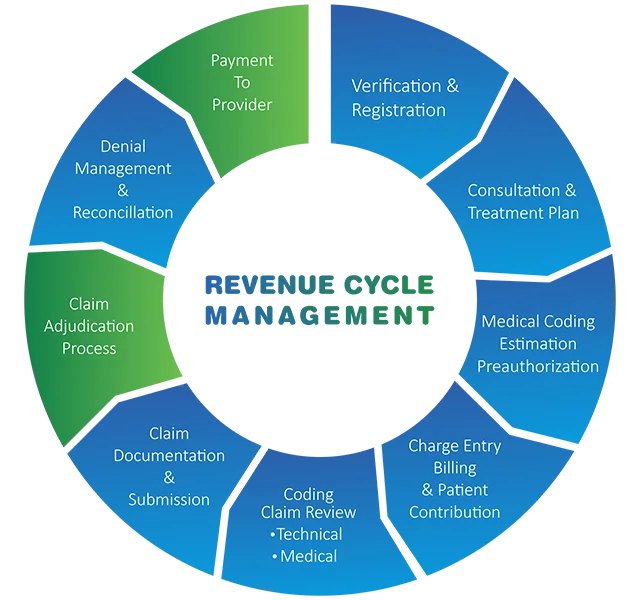
Why Revenue Cycle Management Matters
A strong revenue cycle keeps your organization financially healthy. When eligibility checks, coding, billing, follow-up, and collections are aligned, you reduce leakage and get paid faster.
What We Handle For You
Patient account reviews and billing workflow support
Accurate charge capture and claim submission coordination
A/R follow-up to reduce aging balances
Payment posting visibility and exception handling
Reporting that highlights trends and revenue opportunities
How AM Claims Supports Your Revenue Cycle
We create a reliable workflow across the full billing lifecycle so your team can focus on operations, patient experience, and growth.
Workflow Assessment
We review your current revenue cycle to identify delays, missed charges, and preventable billing issues.
Billing Optimization
Our team improves claim creation and submission workflows for cleaner, faster billing output.
A/R Follow-Up
We actively monitor aging claims and balances to improve collections and reduce outstanding revenue.
Denial Reduction
We flag recurring issues early and support corrective actions that reduce downstream denials.
Performance Reporting
You receive actionable reporting so leaders can track reimbursement health and make better decisions.
Continuous Improvement
We refine processes over time to keep your revenue cycle efficient, compliant, and scalable.

Revenue Cycle Support Built Around Operational Reality
Our team aligns with your workflows and goals, helping you clean up bottlenecks without creating more administrative burden.
Front-End Accuracy
We support cleaner data capture so billing starts with the right information.
Mid-Cycle Visibility
We track claims through adjudication and keep account statuses easier to manage.
Back-End Recovery
We help resolve aging balances, underpayments, and delayed reimbursements more efficiently.

Why Teams Trust AM Claims For Revenue Cycle Management
We combine claims knowledge, disciplined follow-up, and clear communication to help organizations strengthen financial performance over time.
Consistent support across the full reimbursement lifecycle
Practical reporting that helps leadership identify next actions
Experienced teams focused on reducing leakage and delay
Responsive communication that keeps accounts moving forward
Frequently Asked Questions About Revenue Cycle Management
Explore answers to common questions about our revenue cycle management services and how AM Claims supports clients with efficient, responsive claim management.
Our revenue cycle management services can include billing workflow support, claim tracking, accounts receivable follow-up, reporting, and reimbursement improvement strategies.
Let’s Simplify Your Claims Process
Partner with AM Claims for fast, accurate, and compliant claims management across Workers’ Compensation, Pharmacy, and Personal Injury.
